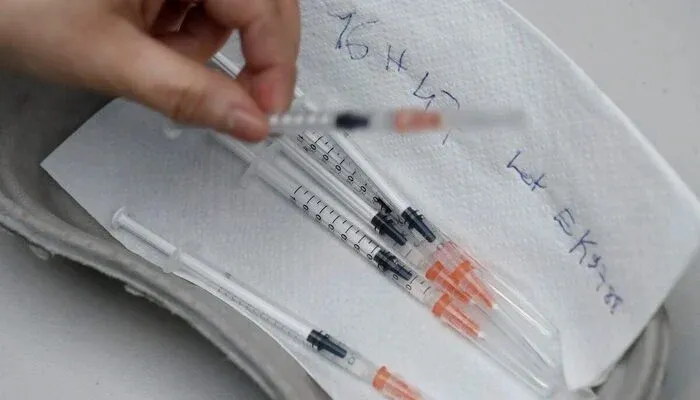
At Dhaka Shishu Hospital, the human cost of Bangladesh’s measles crisis is impossible to ignore. On 7 April, a mother collapsed on the floor, crying for mercy after losing one of her 6‑month‑old twins to the disease. Her surviving daughter lay in the same ICU bed where her sister had died hours earlier. Scenes like this have become tragically common.
Bangladesh is battling one of its worst measles outbreaks in decades, with tens of thousands of suspected cases and hundreds of deaths, most of them young children. Hospitals in Dhaka and across the country are overwhelmed — children lying on floors, oxygen cylinders shared, and wards overflowing.
The resurgence is part of a global trend, but Bangladesh’s crisis is uniquely severe. Experts say it stems from a catastrophic breakdown in vaccine procurement after the 2024 revolution, which disrupted long‑standing arrangements with UNICEF and led to nationwide stockouts. Routine immunisation collapsed, and a major measles‑rubella campaign was cancelled. By late 2025, only around half of eligible children had received their measles shots.
The outbreak began in Rohingya refugee camps in January and spread rapidly, reaching nearly every district. Malnutrition — widespread across Bangladesh — has worsened the death toll, with stunting, wasting and vitamin A deficiency leaving children dangerously vulnerable. Clinics, already underfunded, are struggling to cope.
The newly elected government has moved to restore vaccine procurement through UNICEF and launched emergency immunisation drives targeting millions of children. Vitamin A distribution is set to resume. But health experts warn the virus is spreading too fast for the current pace of vaccination to halt it quickly.
Some are urging the government to declare a public health emergency, arguing that the scale of the crisis demands stronger action.
The political fallout is intensifying. The new administration has blamed both the previous government and the interim authorities for procurement failures. Legal complaints have been filed alleging corruption and mismanagement. Former officials defend their decisions, saying they sought transparency — but acknowledge the human tragedy that followed.
For families like Konika Akter’s, the debate offers little comfort. A disease that Bangladesh once kept firmly under control has returned with devastating force, exposing how quickly public‑health gains can unravel when systems fail.